Although increased direct access to results can be a good thing, we must not forget that there is a big difference between raw results and those interpreted by the person who ordered the test.
There are thousands of laboratory tests, but we as physicians order specific labs to answer specific questions generated by a patient’s history, examination, or personal risk factors, or to monitor ongoing treatments. There are tests that we order in persons who are not having problems to find conditions where early detection matters, such as diabetes or high cholesterol, and even that short list varies by a person’s age, gender, and other factors. Ordering labs without “the contexts” that I described is like going to a restaurant and asking for “something random from the menu”
There is an old fisherman’s phrase about “casting a wide net and seeing how many fish can be harvested.” Some people believe, albeit incorrectly that this is how laboratory tests are utilized (Order lots of them, see which ones are abnormal, and that will tell us what’s wrong with a patient. Or, if they’re all normal, the patient is OK.) That is irresponsible medicine. The true meaning of abnormal and even normal results depends on the question that led to the test of being ordered in the first place.
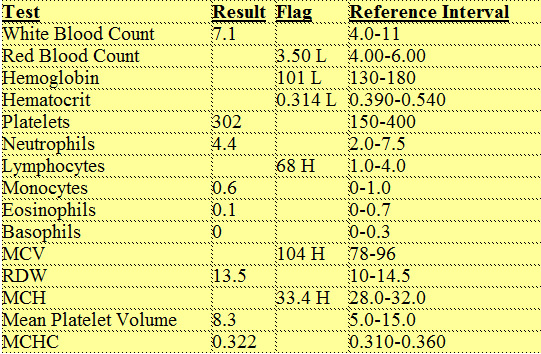
Many patients often attempt to interpret their own labs and ask where do the “H” and “L”’s or the “normal” ranges next to the results come from? Typically, at least once a year, each lab obtains specimens from a group of healthy persons, runs many different tests, and for each test determines a ‘reference range” using statistical calculations. The reference range usually covers the middle 95 percent of healthy persons, meaning that 5 percent of healthy persons will have a result that is above or below the “normal” range. Each lab may have a different reference range for each test. So, having a high or low value doesn’t automatically mean that there is a problem or that there isn’t. This also means that a healthy person has a 1 out of 20 chance of having an abnormal test (a false positive). Often these false positives lead to unnecessary further testing, some of it expensive.
This is why medicine isn’t always linear and also why lab results are best interpreted by a health care provider. By thinking about the question we were trying to answer when we ordered the test as well as knowing the reliability of the test, we can decide when an abnormal test is significant. Some tests are great at ruling out specific conditions, if they’re normal, but not in telling us which of several possible diseases is the cause of an abnormal result, or vice versa. That is why we order tests after deciding what we are looking for rather than indiscriminately ordering lots of tests, and why we need to interpret the results instead of just looking for the “H”s and “L”s. Depending on the situation, a “normal” test can be a sign of the problem.
Here’s a non-medical example of how the same “result” can be interpreted differently, depending on circumstances. You’re home alone late one night in a quiet house, and you hear noise on the street outside. You know that the sound could be from any of a number of things, ranging from the trivial to the serious, so you incorporate additional knowledge to decide how to respond. If it’s a windy day, or it’s a noise that you’ve heard many times and know to be insignificant, you may ignore it. On the other hand, if there have been break-ins in the neighborhood, you may end up calling the police.
A physician’s interpretation of test relies on knowing what each result might mean and using what we know about the patient to draw a conclusion.
There are many potential benefits to patients being in the driver’s seat when it comes to their healthcare and ordering their own labs. However, we can’t forget the value that physicians and other health care professionals bring to the interpretation of laboratory results in support of health care decisions in collaboration with patients.
In health and service,
Dr. Boyce